- VICTORIA KYRIAKIDES: AT THE VANGUARD OF FASHION, IN GREECE AND THROUGHOUT THE WORLD
- Greek-American Cassandra Kulukundis on her 2026 Oscar win for ‘Best Casting’
- IN SERVICE OF THE STATES: GREEKS AT THE BATTLE OF DERNA
- Ancient Greek Theatre (AGT) students of Hellenic Classical Charter Schools in Brooklyn (Park Slope) and Staten Island in Greece!
- From Athens to the world: The artist who draws logic
Dr. George Liakeas on His Miraculous Recovery from The Virus
Dr. Liakeas, 48, is in family practice and the medical director of Lexington Medical Associates in Manhattan. He is affiliated with Lenox Hill and Mount Sinai Hospitals and has been in practice for sixteen years, with a Top Doctors rating numerous times. He is a past president of the Hellenic Medical Society.

DR. GEORGE LIAKEAS
Can you tell me when you got sick and you were admitted?
I first noticed some symptoms on March 20. I was still on the phone with patients who thought they may have a fever of 99′, while I in fact did have a fever of 102′. They were real by the 23rd, but I was admitted on March 25. Ambulance came at 11am and by 1pm I was on the ventilator. Once in the hospital, I very quickly felt like a patient in need of assistance and I remember calling the nurses to tell them that I could no longer breathe well. Aside from a few nightmares that I was paralyzed and helpless, that is the last thing I remember, until waking in the ICU with a profoundly long beard.

How long you were in the hospital?
Fourteen days.
What do you remember of those first days?
Breathe well. That’s the last thing I remember clearly. I was put into an induced coma and placed on a ventilator. I do recall some nightmares of being paralyzed, feeling helpless. When after 11 days, I regained my consciousness and was extubated, I recall touching my chin and feeling heavy beard growth. This was the first realization that I had been wherever I was for a long time.
Your prognosis on admission?
During the intubation, the prognosis, of course, was uncertain and day by day. Some studies have placed the likelihood of my survival as low as 6% and only as high as 20%. The risks while being intubated go past the risk of lung damage, but also to include multiorgan damage.
How long you were intubated?
Twelve days. Luckily after being extubated, my vital signs even without oxygen were as the nurses described “miraculously” better.
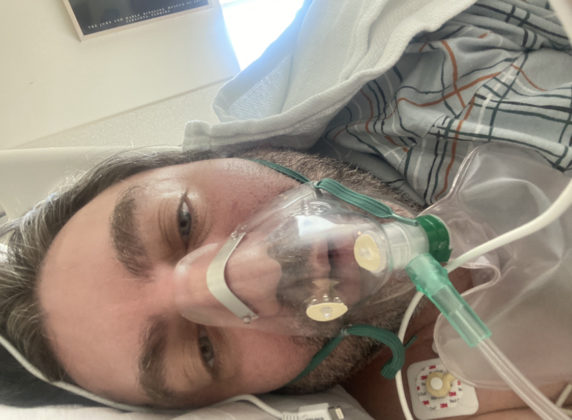
Dr. George Liakeas intubated
When were you released?
April 8. After being extubated, at one point, my cell phone was given to me and as I was sitting there in the darkness, cold and alone, and hundreds of messages which had been stored for two weeks began appearing one by one as if they were sending messages at that moment. Messages came from friends and relatives, but also from patients whose lives I had touched at some point. This was a very emotional moment for me, as I am a person who rarely seeks help, but has taken an oath to give help for a living. The deep heartfelt wishes for what was often described as something, “I deserved for all of the good that I have done as a doctor,” was also when I realized that I could have died.
How do you feel now?
Now even three weeks out it is very difficult to breath. It feels like I have just climbed three flights of stairs at all times. I try to walk as much as I can, but will often throw myself on the couch just to take the weight off my legs, which have become very skinny and weak. It takes an hour just to get dressed/showered in the morning, and I use, of course, a seat in the shower and a walker when walking, just like so many of the patients that I have cared for in the past. I now know what it feels like not only to feel ill, but the humbling experience of needing assistance and having to struggle to accomplish simple tasks. It is even hard to text on the telephone without shaking.

Any lingering effects?
In addition to the very obvious breathing difficulties and total body weakness associated with the muscle atrophy from being paralyzed on the ventilator for so long, I also suffer from frequent headaches and dizziness, as well as a profound numbness and occasional stabbing pain in my legs. I have insomnia, of course, wondering if this will be the night that there is a recurrence of not being able to breathe, to wondering whether or not I will wake up if I go to sleep.
What will your recovery be now?
I get speech therapy weekly and physical therapy three times a week. I grew up in a religious home; I serve my church; I consider myself a faithful and religious person but then and there in the hospital, the fact that people cared took on a religious form. A deeper understanding of the importance of faith and the power of prayer overwhelmed me. Caring and kindness, a basic teaching of our church, will now more than ever be an important part of my life.















0 comments